

Digital implant planning uses cone‑beam computed tomography (CBCT) and intra‑oral scanners to build a three‑dimensional virtual model of the patient’s jaw. By merging DICOM and STL files, clinicians can assess bone volume, density, and proximity to vital structures, then virtually place implants in the optimal prosthetic driven position before any incision. This workflow, supported by AI‑assisted segmentation and predictive analytics, yields millimeter‑level accuracy and reduces the need for intra‑operative guesswork.
Gentle Dentistry of Staten Island embraces a patient‑centered philosophy that prioritizes comfort, transparency, and individualized care. The practice integrates digital planning tools to visualise the treatment plan for patients, fostering informed consent and confidence. AI‑driven risk‑prediction models further personalize monitoring protocols, aligning with the gentle, minimally invasive approach that seeks to limit trauma and accelerate healing.
Predictability is a cornerstone of modern implantology because it directly influences clinical outcomes, patient satisfaction, and long‑term success. Accurate pre‑operative imaging and guided surgery lower the incidence of nerve injury, sinus perforation, and excessive bone loss, while shortening operative time and postoperative recovery. In an era where evidence‑based, data‑driven care is expected, digital planning delivers the consistency and safety that both clinicians and patients demand.
 Full‑mouth digital implant pricing varies widely, but a single‑tooth digital implant—including the 3‑D‑planned implant post, custom abutment, and final crown—typically ranges from $3,800 to $6,500 in the United States (2025‑2026 estimates). The base fee reflects the complete treatment plan, not just the titanium screw, and incorporates CBCT imaging ($300‑$600), intra‑oral scanning, CAD/CAD design, and any required auxiliary procedures such as bone grafts or extractions.
Guided surgery surcharge adds $500‑$1,500 to the overall cost, depending on the navigation system (static guide vs. dynamic navigation) and case complexity. This fee is on top of the base implant price and often includes the fabrication of a tooth‑supported or mucosa‑supported surgical guide.
Additional imaging and auxiliary procedure fees cover the initial consultation ($100‑$350), CBCT scan ($300‑$600), and any necessary bone augmentation or sinus lift, each billed separately. Practices like Gentle Dentistry of Staten Island may bundle these costs and offer financing options, but insurance usually covers the surgical portion while the guided‑technology surcharge is treated as a cosmetic or advanced‑technology fee.
 CBCT and intra‑oral scanning integration Modern implant workflows start with a low‑dose, high‑resolution CBCT scan that captures the jaw’s bone volume, density, and proximity to vital structures. Intra‑oral scanners then generate a highly accurate STL model of the dentition and soft tissues. Merging the DICOM (CBCT) and STL (scan) data creates a unified 3‑D patient model that serves as the foundation for all subsequent planning steps.
Software‑based implant positioning Using AI‑enhanced planning software, the clinician virtually places each implant, adjusting depth, angulation, and diameter to achieve optimal bone support and aesthetic alignment. The system can automatically segment anatomical landmarks, suggest implant size, and predict risk factors such as peri‑implant bone loss. This backward, prosthetically driven planning allows the final restoration to be visualized early, ensuring the implant trajectory respects a 2 mm safety zone from nerves, sinuses, and other structures.
Creation of surgical guides The virtual plan is exported to design a patient‑specific surgical guide—either tooth‑, bone‑, or mucosa‑supported—fabricated by 3‑D printing or milling. The guide’s titanium sleeves control drill depth and angulation, translating the digital plan into the clinical reality with sub‑millimeter accuracy. Guided surgery reduces operative time, eliminates flap elevation, and lowers postoperative discomfort, delivering predictable, patient‑centered outcomes at Gentle Dentistry of Staten Island.
Key questions answered
Guided vs. non‑guided implant surgery Guided implant surgery integrates CBCT imaging, intra‑oral scanning, and computer‑aided design to produce a patient‑specific 3‑D printed surgical guide. This guide directs the drill to the planned trajectory, achieving sub‑millimetre placement accuracy and often allowing a flapless, minimally invasive approach. In contrast, free‑hand placement relies on the clinician’s visual and tactile cues, typically requiring larger flaps, more drilling steps, and yielding greater angular variation. Clinical studies report a failure rate of roughly 2 % for guided surgery versus 6 % for non‑guided techniques, translating into higher long‑term survival and more predictable aesthetics. While guided protocols incur additional costs (≈ $500–$1,500 per implant for imaging, software, and guide fabrication), they can reduce the need for extensive bone grafting, shorten chair‑time, and enable immediate provisionalization, offering a favorable cost‑benefit balance for complex cases.
Is digital guided implant surgery accurate and reliable? Evidence shows mean linear deviations of about 0.5 mm at the entry point and 0.8 mm at the apex, with angular deviations under 5°. Dynamic navigation systems further improve precision, achieving coronal deviations below 1 mm and angular errors under 3°. These accuracy metrics correlate with survival rates of 96 %–100 % in systematic reviews and lower incidences of cortical perforation, nerve injury, and postoperative complications.
BioHorizons guided implant surgery BioHorizons combines its proprietary implant platform with a sophisticated digital planning suite. The Pro Surgical System provides a color‑coded, keyless drilling protocol and interchangeable length‑specific drills that work with both guided and free‑hand approaches. A custom surgical guide translates the virtual plan to the mouth, delivering predictable, accurate placement while reducing surgical time and enhancing aesthetic outcomes. Integrated photogrammetry and CAD/CAM workflows streamline communication between the virtual plan and clinical execution, aligning with Gentle Dentistry’s patient‑centered, gentle‑care philosophy.
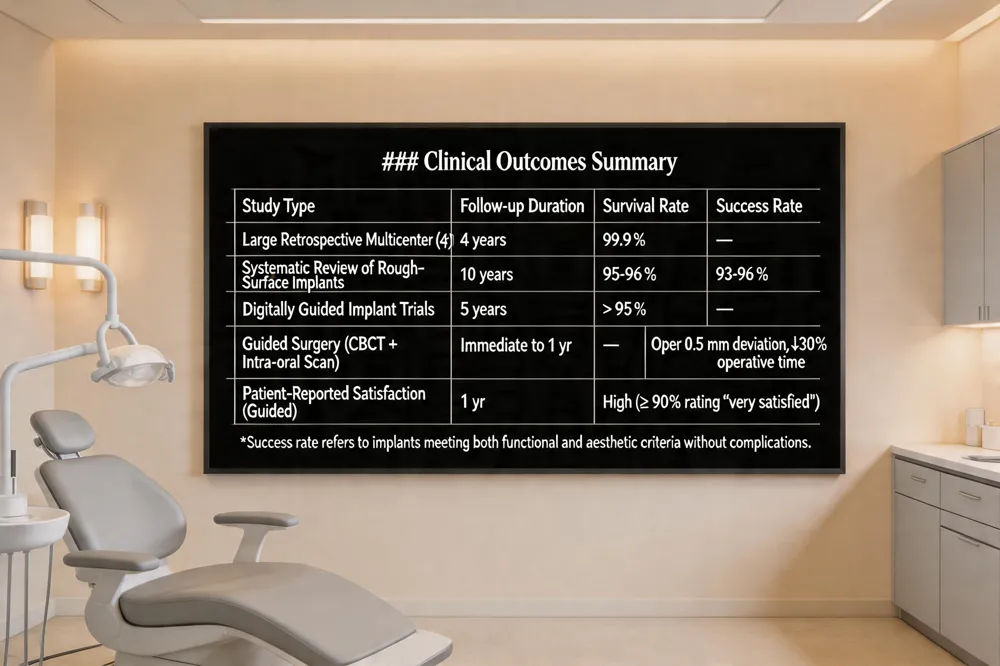 Long‑term survival data for dental implants are consistently high. Large retrospective multicenter studies report an overall survival of 99.9 % over four years, while systematic reviews of screw‑type, rough‑surface implants show a 10‑year implant‑level success of 93 %‑96 % (average ≈ 95 %). Recent clinical trials of digitally guided implant placement demonstrate five‑year survival exceeding 95 % and patient‑reported satisfaction, with minimal postoperative discomfort. Guided surgery using CBCT and intra‑oral scans improves accuracy (often < 0.5 mm deviation) and reduces operative time by up to 30 %, supporting predictable outcomes in practices like Gentle Dentistry of Staten Island.
Numerous clinical trials are actively evaluating implant technologies. Researchers are testing AI‑driven planning, novel surface coatings, adjunctive biologic therapies, and magnetic‑field stimulation to enhance osseointegration and reduce peri‑implant inflammation. In 2025, trials focus on bone‑augmentation methods, AI navigation, dual‑cantilevered single‑implant bridges, and the comparative accuracy of digital versus conventional impressions. These studies are registered on ClinicalTrials.gov and can be filtered by location, phase, and design.
Patients seeking free implant trials near Staten Island should search ClinicalTrials.gov with their zip code or consult the NIDCR trial finder. Local academic centers such as NYU College of Dentistry often sponsor studies that cover implant costs for eligible volunteers. Our office can assist in identifying and enrolling in appropriate trials, ensuring you benefit from the latest evidence‑based implant care.
 Smoking is consistently identified as the #1 risk factor for dental implant failure. Nicotine and other toxicants impair blood flow, diminish bone healing, and increase the incidence of peri‑implantitis and early loss. Patients who quit before surgery and remain smoke‑free during osseointegration experience dramatically higher success rates.
Autoimmune diseases do not automatically preclude implant therapy, but they can affect healing. Careful assessment of disease activity, medication (especially immunosuppressants), and overall systemic health is essential. With disease control, thorough pre‑operative planning, and close postoperative monitoring, successful outcomes are achievable.
The "3‑2 rule" is a prosthetically driven guideline that mandates at least 3 mm of buccal bone thickness and 2 mm of soft‑tissue (gum) between the implant and adjacent teeth. This ensures adequate biological width, prevents dehiscence, and promotes a natural emergence profile, especially in aesthetic zones.
By recognizing smoking as the dominant risk, evaluating autoimmune status, and adhering to the 3‑2 rule, clinicians can enhance patient safety, reduce complications, and achieve predictable, long‑term implant success.
 The gentle‑care philosophy at Gentle Dentistry of Staten Island begins with clear communication: 3‑D visualizations of the digital workflow let patients see the planned implant position, prosthetic design, and final smile before any incision, fostering confidence and informed consent. Nutrition after digital dentures is straightforward—soft foods such as soups, scrambled eggs, and yogurt are ideal during the first week, while warm‑water rinses and gentle brushing keep the prosthesis clean. As oral muscles adapt, patients can gradually reintroduce firmer foods, always avoiding very hard, sticky, or chewy items that might fracture the denture. Healing and comfort are enhanced by minimally invasive, flapless guided surgery, which reduces tissue trauma, postoperative swelling, and pain, often allowing same‑day provisional crowns. AI‑driven planning predicts optimal implant placement, further minimizing complications and supporting a swift, comfortable recovery. Together, these digital tools deliver a predictable, patient‑centered experience that aligns with the practice’s commitment to personalized, gentle implant care.

AI transforms dental implantology through diagnostics, planning, navigation, and follow‑up.
Supervised learning predicts peri‑implant bone loss, implant failure, and sinus augmentation needs, while CNNs analyze radiographic and CBCT images with >90% accuracy for disease detection.
AI diagnostic models identify marginal bone loss and peri‑implantitis early, supporting earlier intervention; Prognostic AI assesses individualized risk using systemic health, bone quality, periodontal history, and implant parameters, with Neural networks achieve up to 94% predictive accuracy for single‑implant success.
Interpretability challenges require explainable AI such as saliency maps and feature importance rankings; many AI models function as ‘black boxes’, prompting the need for explainable AI techniques such as saliency maps and feature‑importance rankings.
Future research must focus on standardizing imaging protocols, creating large, demographically diverse training datasets, and conducting prospective multicenter clinical trials to ensure generalizability and reduce algorithmic bias (Future directions: explainable AI, standardized imaging, large diverse datasets, prospective multicenter trials).
External validation on diverse data sets will improve calibration, allowing AI predictions to be trusted in everyday clinical decision‑making and to align with the patient‑centered, gentle dentistry philosophy (Clinical utility depends on calibration, real‑world impact, and clinician‑centered workflows; AI aligns with Gentle Dentistry’s patient‑centered, personalized implant care.
 Gentle Dentistry of Staten Island follows an end‑to‑end digital process that begins with a low‑dose, high‑resolution cone‑beam CT (CBCT) and a precise intra‑oral scan. The two data sets are merged into a single 3‑D patient model, which AI‑assisted planning engines analyze to suggest optimal implant size, angulation, bone density, and any need for sinus augmentation or grafting. The virtual plan is reviewed with the patient using 3‑D visualizations, allowing clear, patient‑centered communication and informed consent. Once the prosthetically driven plan is approved, a custom surgical guide is fabricated through CAD/CAM or 3‑D printing, incorporating titanium sleeves for depth and angulation control. During surgery the guide is seated tooth‑ or mucosa‑supported, enabling flapless, minimally invasive placement with sub‑millimeter accuracy and reduced operative time. Provisional restorations can be milled or printed and placed the same day, while the final crown is fabricated after osseointegration. Throughout the workflow, the practice emphasizes gentle techniques—low radiation exposure (ALADAIP), minimal tissue trauma, and rapid recovery—while maintaining predictability and comfort. This integrated, AI‑enhanced digital workflow not only streamlines clinical steps but also builds patient confidence through transparent visual planning, ultimately delivering lasting, aesthetically pleasing implant outcomes.
Digital and AI‑enhanced implant workflows have transformed predictability in modern implant dentistry. High‑resolution CBCT combined with intra‑oral scanning creates a 3‑D model that allows clinicians to map bone volume, nerve pathways, and sinus anatomy with sub‑millimeter precision. AI‑driven segmentation and prosthetically‑driven planning automate bone segmentation and optimal implant positioning, while computer‑guided surgical guides translate the virtual plan into a physical guide that consistently achieves deviations under 0.5 mm and angular errors under 3°. Clinical evidence shows survival rates of 96‑100 % and marginal bone loss often below 0.5 mm when guided, flapless techniques are employed, confirming that digital planning reduces intra‑operative guesswork, surgical time, and postoperative complications.
These technological advances align perfectly with a patient‑centered, gentle approach: patients view 3‑D visualizations of the final restoration, experience minimally invasive surgery with reduced swelling, pain, and chair‑time, and benefit from personalized risk assessments powered by AI. The result is enhanced confidence, faster recovery, and long‑term functional and aesthetic outcomes.
Gentle Dentistry of Staten Island invites you to schedule a consultation to experience these state‑of‑the‑art, predictable, and compassionate implant solutions tailored to your unique anatomy and goals.